- What is ankle instability?
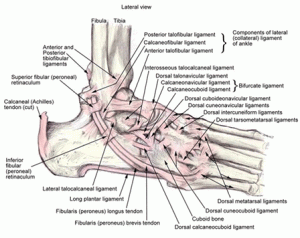
Its exactly as it sounds – an ankle that is unable to maintain stability through normal usage, resulting in pain, recurrent sprain, falls, or a combination of the above. There are three groups of ligaments on the outside of the ankle – the anterior and posterior talofibular ligaments (ATFL and PTFL) and the calcaneofibular ligament. A simple sprain/strain will always tear the ATFL; a more severe sprain will also involve the CFL. The PTFL is rarely involved unless there is also an ankle fracture or a frank dislocation of the ankle.
Often I will have patients come to see me 4-6 weeks after their sprain, with a MRI reporting “a 100% tear of the ATFL”. This sounds very impressive, but really this is just what a sprained ankle actually is. I would only be looking at a surgical solution for someone who was having frequent sprains/strains/falls with minimal trauma, or they’d had 6-9 months of physiotherapy with no improvement.A simple ankle sprain (by simple I mean no cartilage, bone or tendon damage) should heal, if given enough time, and particularly if it’s the first or second sprain. But the trick is enough time – a well-sprained ankle can take up to six months to full rehabilitate. Not that it will be unstable for this period, but the patient will have pain, swelling and feelings of instability, without actually falling. The time factor is key – it will usually be feeling pretty good at 6-8 weeks post-injury, but will have an increased risk of injury if stressed.Often the people who come to surgery will have a severe, yet simple sprain; have standard nonoperative treatment (RICE), and go back to normal activities too early – and they roll it again. And again . . . and again. Each time they roll it more easily; each time they lose some function that they don’t get back.
- MRI
This is really the investigation of choice if surgery is planned. It will be able to diagnose which ligaments are involved, and how functional they may be; it can check for an cartilaginous damage on either the talus or tibia; and look for any tendon damage that may change the surgical plan.
- How should a simple sprain be treated?
Well, simply . . . Rest, Ice, Compression, Elevation . . .in other words, stop trying to run on it but keep it moving! Perhaps you might go in to a surgical boot or a cast for a week or two if its extremely painful or swollen, but you have to move it.
Physiotherapy is vital, as they are very helpful in terms of swelling control, and monitoring progress. Nonoperative treatment of simple sprain is well-accepted, and the majority do extremely well.
- Who should have an operation?
Unless there is a co-existing cartilage injury ie a loose body in the ankle, or something similar; it should really only be someone who has true ankle instability, which is confirmed by clinical examination and preferably MRI findings. If the patient has a positive MRI, but the ankle feels stable to examination and the patient really only has pain, then they are going to be pretty unhappy with an ankle stabilization procedure.
- What surgery should I have?
If your ankle is unstable enough to be talking about surgery, you should have an operation that stops that. This sounds obvious, but there are a lot of described operations that won’t necessarily allow normal, full-contact use of the ankle even though they are considered reconstructions.
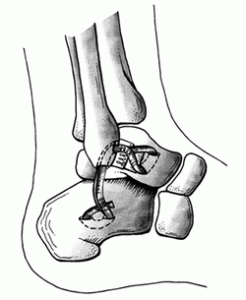
I mostly do an operation that while it doesn’t reproduce the normal anatomy, leaves the ankle stable and usable after rehab has been done. I harvest the gracilis tendon (one of the hamstrings) from behind the knee (the same one that can be taken for ACL reconstruction), and reroute it through a tunnel in the fibula, plugging it in to the talus and calceneus. This is by no means something I have invented, but rather adapted from some existing operative descriptions. This reconstructs the ATFL and CFL, which are the ligaments involved. I deliberately don’t create a bony tunnel in the talus, as I believe the risk of talar damage (avascular necrosis) is too high, when I can tunnel it through the soft tissues for a similar outcome.
Believe it or not, the gracilis tendon mostly reforms. It is one that is harvested quite commonly in knee ACL reconstructions, and by the time you are ready to run, your hamstrings will have recovered.
The surgery is technically fairly simple, but the rehab afterwards is very time consuming, and the result you get will definitely hinge on the amount of work you put in to it.
You will be nonweight-bearing in a cast and surgical boot for three weeks; you can then walk in the boot for another three weeks; then the boot is weaned off over a two week period, and the real rehab begins. You are really looking at 4-6months postop until you can run comfortably . . . but this is how long it takes for it to heal properly and get your function back. - But what if I have pain, a positive MRI but my ankle feels stable?
This is a very difficult situation; and the worse thing to do is to rush in to an operation in the absence of true instability. There is likely to be an element of a chronic pain syndrome, scar tissue in the joint and maybe even early arthritis, and the treatment may not end up being surgery. I will say it again – if your ankle is not unstable to examination, despite what a MRI may say, you will not be happy with reconstruction surgery. Anyone who guarantees you anything with surgery, particularly foot and ankle surgery, is perhaps confused and you should see someone else.

Dr Shooter – Arthroplasty Practice
save life, save limb, restore function